
Nowadays, osteochondrosis is rightly considered "the disease of the century" because it most often affects people whose work does not require increased physical activity.
In most cases, changes in cartilage and bone tissue are seen in people of working age, up to 40 years old.
The disease can affect different parts of the spine, and the second most common is cervical spine osteochondrosis.
What's this?
Osteochondrosis is a degenerative disorder of articular cartilage and adjacent bone tissue.
The term was previously used for a large group of osteoarticular diseases, but is now used only for degenerative diseases of the spine.
Compared to other parts of the spine, the cervical region is the most mobile, with many nervous and vascular formations. The structure of the vertebrae is small, as well as the fact that they are surrounded by a rather weak muscle ligament.
This anatomical structure predisposes to the development of osteochondrosis, the severity of the clinical manifestations of which depends on the nature of the changes in the intervertebral discs and the extent of their destruction.
Causes of the disease
The main and most common cause of osteochondrosis of the cervical spine is a sedentary lifestyle.
Due to lack of physical activity associated with a sedentary and sedentary lifestyle:
- metabolic processes are disrupted;
- increases salt levels in the bloodstream and lymph fluid;
- Salts are deposited in the cervical spine, kidneys and liver.
Damage to the cervical vertebrae is primarily caused by a lack of nutrients in the intervertebral discs. Therefore, improper and unbalanced diets are among the main causes of osteochondrosis of the neck.

Risk Factors
There are several risk factors for cervical osteochondrosis.
The most common factors are:
- inheritance;
- age-related changes; cervical spine
- injuries;
- hypothermia;
- hormonal disorders that lead to metabolic disorders;
- some autoimmune diseases that damage cartilage tissue (systemic lupus erythematosus, rheumatism).
Why is it dangerous?
Not only the spinal cord and nerve roots pass through the cervical spine, but also the vertebral artery, which is responsible for the blood supply to the back of the brain, the medulla oblongata, and the cerebellum.
Therefore, in cervical osteochondrosis, this artery is compressed and, as a result, the cerebral circulation is damaged.
In extremely advanced cases, compression of the artery, adjacent blood vessels, and nerve plexuses can lead to consequences such as:
- lack of coordination;
- hearing and vision loss;
- stroke.
If the disease does not heal in the initial stage, it can lead to complications such as: protrusion of the intervertebral disc or herniated disc.
Progression of the disease
Cervical osteochondrosis, like osteochondrosis of other parts of the spine, develops intermittently. There are 3 stages in the development of the disease.
1 degree
Characterized by the onset of destruction of intervertebral discs.
Cracks form in the annulus fibrosus, the strength and elasticity of the disc are disturbed, its height decreases, causing the nerve roots to compress.
Typical aching pain appears. Sometimes in stage 1 (preclinical) such pain may be absent and osteochondrosis is associated with moderate discomfort in the neck.
Grade 2
If grade I osteochondrosis has not been treated or treatment has not been effective, a chronic condition occurs, which is stage 2 osteochondrosis.
The pain becomes constant, the destruction and compression of the intervertebral disc continues, and leads to minor dislocations of the cervical vertebrae.
At this stage, cervical osteochondrosis may develop a decreasing head syndrome. This syndrome is characterized by severe pain and the person needs to keep their head fixed to reduce the pain.
Grade 3
Grade 3 cervical osteochondrosis has the following symptoms:
- headache;
- nausea;
- dizziness;
- neck "lumbago";
- Decreased sensitivity of the upper limbs.
The annulus fibrosus is almost extinct, leading to complications of osteochondrosis - prominence of the intervertebral disc or intervertebral hernia.
In stage 3 osteochondrosis, the intensity of the pain may decrease because the affected cartilage tissue of the intervertebral disc simply does not exist, which means that there is no source of pain but the pinching of the nerve roots remains, so the pain does not go away.
Signs and Symptoms
There are many signs of this disease. And they depend on which vertebrae are damaged by this disease.
Typical syndromes of cervical osteochondrosis:
- radical syndrome;
- vertebral artery syndrome;
- cervical migraine syndrome;
- hypertensive syndrome.
All of these syndromes are primarily accompanied by different types of pain.

If we consider the vertebral artery syndrome, then here the headache manifests itself at an early stage in the development of the disease.
In this case, the pain attacks may be accompanied by:
- dizziness;
- unsteady gait;
- visual symptoms (appearance of fog in the eye, decreased visual acuity, etc. ). fainting (with sudden head movements).
In hypertensive syndrome, increased intracranial pressure is defined.
Headaches are more explosive and may cause nausea and vomiting. As cervical osteochondrosis worsens, an increase in temperature and an increase in ESR are observed.
When the roots of the spine are compressed ("radicular syndrome"), the following neurological symptoms may occur:
- severe pain in the neck (cervicalgia);
- neck pain extending to the forearm and humerus (cervicobrachialgia);
- pain in the arm;
- crack or crack in the neck when the head is turned;
- "radiant" pain in the ear, which most often occurs after a long, uncomfortable position or sudden movement;
- feeling of pain or lump in the throat, breathing problems;
- numbness of the hands and tongue;
- feeling of swelling of the tongue;
- severe weakness;
- hearing and vision impairment;
- tinnitus;
- general deterioration of health.
In "cervical migraine" syndrome, irritation of sympathetic nodes is observed, leading to disruption of cerebral vascular reactivity and damage to blood circulation.
This can lead to hypertension, which can often be accompanied by:
- stuffy ears;
- tachycardia;
- noise in the head;
- rings in the ear.
When the arteries that supply the spinal cord are compressed, a spinal cord stroke can occur.
Impairment of cerebral circulation in osteochondrosis can cause:
- lack of oxygen in brain cells;
- mental disorders (depression, panic attacks);
- Signs of epilepsy, such as short-term loss of consciousness and tension all over the body - these are often confused with signs of epilepsy.
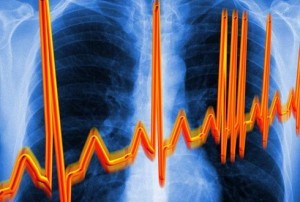
Cervical osteochondrosis is a very common sign of changes in heart rhythm and disorders such as extrasystole or arrhythmia.
These symptoms are very common among drivers and office workers.
Due to the sedentary lifestyle, changes occur in the intervertebral discs of the cervical and thoracic spines that lead to disturbances in the work of the heart.
In most cases, until osteochondrosis is cured, it is virtually impossible to get rid of arrhythmias.
Edema under the eyes may also indicate osteochondrosis of the cervical spine.
They most often depend on the position of the head during sleep at night, disappear during the day, and cause headaches, dizziness, headaches, and so on.
Vegetovascular dystonia is the other most common disease that occurs with this disease.
Consequence of trapped vessels running along the side of the spine.
Diagnostic Methods
Preliminary diagnosis is made by a neurologist during the patient's first examination. More recently, the doctor had to diagnose by performing only an external examination of the patient and sending it for an x-ray.
But unfortunately it is impossible to see the full picture of the development of the disease on an X-ray.
Studies such as computed tomography and magnetic resonance imaging are currently available to fully assess the stage of the disease.
After the diagnosis is made, the patient is referred to a doctor who specializes in this area.
Which doctor is treating you?
Treatment is performed by a specialist with a narrow focus - a vertebrologist or a vertebroneurologist.
Treatment of cervical osteochondrosis
The severity of the main clinical symptoms is based on the treatment of cervical osteochondrosis.
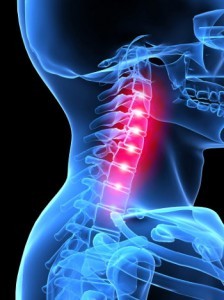
In the cervical spine, symptoms are primarily associated with constriction of blood vessels and nerve endings, so during treatment, above all, edema is removed and blood circulation is restored.
A number of treatments are used to treat cervical osteochondrosis.
The most effective treatment is the complex, which is a combination of several conservative treatment methods.
Complex treatment of cervical osteochondrosis may include the following traditional and non-traditional methods: medication, massage, acupressure, manual therapy, physiotherapy, acupuncture, homeopathy, folk remedies, etc.
The main stages of treating osteochondrosis are the same for all localizations of the disease:
- You need to relieve the pain first.
- The swelling then disappears.
- At this stage, blood circulation should be normalized.
- Strengthening the muscle ligament.
- Improving nutrition and tissue regeneration.
Only a team of good professionals can select the most appropriate therapy, which includes a neurologist, physiotherapist, massage therapist, surgeon, and vertebral neurologist.
Like all diseases, cervical osteochondrosis should be treated at the earliest stage of its onset. If you do not start the process, you can achieve complete recovery from osteochondrosis at this stage.
Unfortunately, stages 2 and 3 of cervical osteochondrosis are accompanied by complete or partial destruction of the intervertebral discs, so these stages are characterized by a very long recovery process.
First Aid
How to relieve pain during exacerbation?
In case of severe pain, you need to take painkillers from your home doctor's office: these can be painkillers. You can also use pepper plaster for pain.
Diuretics may be taken if swelling occurs. Rubbing the neck with analgesic ointments can help.
You can also use theneedle applicatorfor pain relief, which:
- relieves back pain;
- reduces muscle cramps;
- stimulates the work of internal organs;
- normalizes blood circulation.
Physiotherapy in exacerbations is contraindicated, as well as warm-up, as these effects can cause serious complications.
After relieving acute pain, you should consult your doctor immediately.
Medication
Medication usually starts with injections (in case of worsening) and is then switched to tablets and suppositories in combination with topical ointments and gels.
Anesthesia is performed with steroidal anti-inflammatory drugs during medication.
Medications that restore cerebral circulation should be prescribed.
Muscle relaxers may be prescribed for abnormal muscle tension. For more effective treatment, vitamins are taken in therapeutic doses and trace elements.
Surgery is often recommended for intervertebral hernia and your doctor may recommend surgery.
Massage and self-massage
This method works well with physiotherapy and physiotherapy. You can take a massage course at any medical institution and also contact private clinics.
Massage is required for osteochondrosis of the cervix to strengthen the muscles and release neck tension.
The task of the masseur is to remove harmful metabolic products by increasing the outflow and inflow of blood in the diseased area and to remove the spasm from the diseased area.
The main techniques used by neck massage professionals are:
- caressing;
- squeezes;
- rubbing;
- vibration;
- kneading.
The self-massage technique can be performed using the following techniques:
- stroking (movements should be soft, without much effort, forming folds)
- kneading (deep effect on the muscles, by gripping, pushing and pushing into the shoot);
- vibration (vibration shock, shaking, tapping).
Self-massage should always be completed by stroking. You can use a massager while vibrating.

Acupressure Massage
Acupressure massage relieves headaches by worsening cervical osteochondrosis, helps pressure waves, and normalizes them.
Acupressure Scheme:
- Effect on the feng fu point below the occipital bulge for 1 minute.
- Effect on the feng chi point, which is located two fingers from the mastoid processes of the skull.
- Effect 1-1, 5 minutes on the ya-men point (which is three fingers from the feng fu point).
- Sedation 1-1, 5 minutes at da-chzhui point (7th cervical vertebra).
You should lie down for a few minutes after acupressure as you may experience mild dizziness.
Manual therapy
Manual therapy helps to cope with both acute and chronic pain, increases range of motion and also improves posture.
Main methods of manual therapy for cervical spinal osteochondrosis:
- Relaxing and segmental massage.Used to warm up muscles and relieve tension.
- Mobilization.Effects of restoring joint function by traction.
- Manipulation.A sharp push to the patient's abnormal areas. The procedure is accompanied by a characteristic cracking (return of the joint to its normal position).
These techniques should be handled fluently by a practitioner of manual therapy. Otherwise, any error may result in injury.
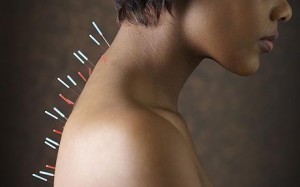
Acupuncture
Acupuncture promotes the release of cortisol into the bloodstream. This hormone has a pronounced anti-inflammatory effect.
Acupuncture is performed by acting on points near the inner edge of the scapula. The needles are inserted to a depth of 1-2 cm and left to act for 10-30 minutes.
Homeopathy
Medication has a number of harmful side effects, so homeopathy can be a worthy substitute for treatment without the unintended consequences.
Nutritional characteristics
Food should be rich in calcium and magnesium.
These trace elements are found in fish and seafood, nuts, legumes and dairy products.
Osteochondrosis of the neck can often be accompanied by atherosclerosis. In this case, a strict diet is recommended.
The diet is prescribed for 3-4 months. Consumption of all cholesterol-containing foods should be restricted. These include animal fats, fatty meats, fatty dairy products, etc. You should also limit or exclude the consumption of salt, sugar, flour products.
It is advisable to give up bad habits (smoking, alcohol, etc. ).
Cervical osteochondrosis and alcohol are associated. The fact that when it enters the blood, alcohol destroys the cells, thereby aggravating the already damaged blood circulation in osteochondrosis.
Therefore, you should keep it to a minimum and stop drinking it completely when it gets worse.
Disease Prevention
To prevent cervical osteochondrosis, it is recommended that you follow these rules:
- Sleeping
- should be on a solid mattress and on a low cushion: the bending angle of the neck should not exceed 15 degrees;
- take a hot shower every day for at least 10 minutes;
- visit the sauna and bath as often as possible: the heat helps to relieve neck cramps;
- give yourself aerobic activity and regular walks at a low pace;
- swim;
- Avoid spine shock loading (jumping, running) after 25 years;
- When doing sedentary work, be sure to take five-minute breaks per hour;
- regular yoga practice can prevent any manifestation of cervical osteochondrosis;
- refuses to go to the gym as bodybuilding can cause the cervical disc to protrude;
- Exercise, like preventing osteochondrosis of the neck, helps strengthen the neck muscles, relieves tension.
Frequently Asked Questions
What to do during pregnancy and how to treat it?
The first symptoms of osteochondrosis of the neck often occur during pregnancy.

This is due to changes in hormonal levels and softening of the vertebrae, as well as displacement of the center of gravity and excessive stress on the spine.
Treatment of osteochondrosis in pregnant women is quite complicated because it is mainly limited by the pharmacological method of analgesia.
You can apply natural ointments or use traditional medicine.
Any effect on the neck area during pregnancy (warm-up, exercise, etc. ) is strictly prohibited.
Does it occur in children and adolescents?
In children and adolescents, cervical osteochondrosis develops due to congenital or acquired functional insufficiency of cartilage tissue.
Expresses complaints of headache, fatigue, dizziness, and fainting.
Can the neck area be heated?
Warming of the neck is strictly prohibited in cervical osteochondrosis, especially during the exacerbation phase of the disease, as warming up can lead to an increase in edema and vasodilation.

How to sleep properly?
Sleep on a flat, hard bed with an orthopedic mattress.
The recommended and most comfortable posture lies on your side, your shoulders on the mattress and your head resting on a small pillow.
The use of an orthopedic pillow relaxes the muscles of the cervical spine, reduces irritation of nerve endings, which prevents headaches and insomnia.
Is physical activity and sauna allowed?
In preventive measures and in the first stage of cervical osteochondrosis physiotherapy exercises, swimming is recommended.
Weight lifting, hard work, gym training is strictly forbidden.
A visit to the spa and sauna is also only recommended for the prevention of cervical osteochondrosis and in the early stages of the disease.
Reviews
"I would like to share with my unfortunate siblings how to treat cervical osteochondrosis. I had back pain a few years ago. A visit to the doctor, the diagnosis was cervical osteochondrosis. I tried a lot ofwas also a very expensive procedure. I had to start a thorough study of the problem. So I decided to try swimming. It has been found that swimming is widely used for the prevention and treatment of osteochondrosis of the neck as it relieves tension in the neck muscles. pool and grief I don't know. "
"Because of my overwork, I couldn't find time to see a doctor. And my relatives advised me to treat my neck pain with warm-ups, herbal compresses, various ointments and other home remedies. That my neck stopped at all! I lay at home for more than two weeks thenI have also recovered for a long time, so I advise everyone to see their doctor as soon as their neck cracks and hurts! So it saves time and does not lose your health.



























